Responsive neurostimulation (RNS) is a breakthrough surgical approach to treating seizures that are not controlled by medication. A neurostimulator is placed under the scalp and within the skull, and it is connected to 2 electrodes placed either on the surface of the brain, into the brain, or a combination of both. The device continuously monitors brain activity and then is programmed to detect seizures. When a seizure or seizure-like activity is detected, the device delivers a small amount of electrical current to the brain to stop or shorten the seizure, or possibly prevent a seizure altogether.
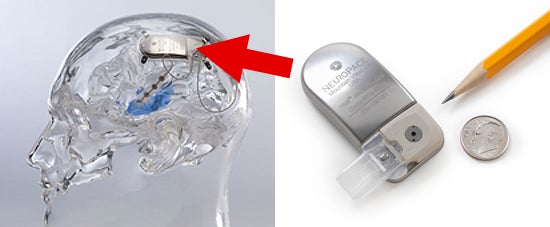
Who should get RNS?
The RNS system is used to treat adult patients with focal epilepsy who have failed treatment with at least 2 seizure medications. Our approach is always first to determine whether patients are candidates for resection of their seizure focus, the only potential cure for epilepsy. Patients are considered candidates for RNS when they have undergone comprehensive diagnostic testing that has localized one or two seizure foci, but are determined not to be candidates for surgical resection for a particular reason. These reasons include seizures that originate from more than one area of the brain, seizures that arise from areas of the brain that cannot be safely resected, or seizures that are difficult to discretely localize.
[See newspaper article from the Tribune-Review on McCandless woman 1st in region with implant aimed at halting seizures.]
How does RNS work?
RNS is a “closed loop” system that continuously monitors the brain’s electrical activity and sends a brief pulse of electrical stimulation directly to the brain when a seizure or seizure-like activity is detected. Doctors specially trained in RNS program the neurostimulator and gradually train it to detect specific patterns unique to a patient’s seizure.
How effective is RNS?
In clinical trials, more than half of the patients treated with RNS had 50% or fewer seizures compared to their presurgical baseline. The median decrease in seizure frequency with treatment was:
67% at 1 year
75% at 2 years
82% or more in years 3 through 6
Perhaps more importantly, most patients reported significant improvement in their quality of life with RNS.
It is important to keep in mind that seizure reduction from RNS is not immediate. It may take several months to notice an improvement, and it will likely take years to achieve the optimal results.
What is the surgery like?
Surgery to implant the RNS system is performed under general anesthesia and typically takes between 2-4 hours. Many patients are able to go home the next day, and others can expect a 1-3 day hospital stay. No bed rest is required after surgery, and many patients are able to return to their daily activities within a few days and even return to work in 2-4 weeks.
What are the patient responsibilities with RNS?
Patients who choose treatment with the RNS system play a key role in their own care. Each patient is given a remote monitor, which is essentially a laptop computer, to which they must download the information stored on their neurostimulator on a daily basis. This process takes just a few minutes a day. Once a week, they are asked to upload the data stored on their remote monitor to a secure website database where their doctors can review it. Patients are given a magnet and are asked to swipe the magnet over their neurostimulator when they have a seizure. This action marks that particular event as important, and the device stores the brain activity recorded during that time so the doctor can take a closer look at it. It is also very helpful for patients to keep a detailed journal noting when they have a seizure. It is extremely important that the patient be willing and able to attend the follow up appointments so the device can be programmed as needed to achieve the best results. Typically, follow up appointments are scheduled every 4-6 weeks throughout the first year, but eventually become less frequent.
