The management of adult spinal deformity remains a challenging and controversial endeavor. It is estimated that adult degenerative scoliosis affects greater than 15% of the current United States population older than 60 years of age. The need for evidence based strategies to care for this condition has intensified as the baby boomers age and the prevalence of this condition continues to mount. In the current health care environment, with cost containment and resource limitations, physicians have had to develop new ways to treat this growing problem with a “less is more” approach. At UPMC, we have developed a treatment strategy to this debilitating condition where in fact we can achieve “more with less”—less invasive that is.
Adults with spinal scoliosis typically present with chronic back pain due to asymmetrical degeneration of the spine. They can also have associated leg pain or weakness caused by the concurrent narrowing of the spinal canal and nerve root exit holes that contemporaneously occurs with the structural deformity. Conservative management under the guidance of a spine care professional is the mainstay of treatment for this condition, yet its efficacy is limited in both its functional as well as its aesthetic value. Although there is no consensus as to the optimal surgical management of spinal deformity, those treated operatively have shown a significantly greater improvement in their pain and overall quality of life when compared to their non-operative equivalents.
When symptoms remain progressive and refractory to conservative treatment, surgical correction is considered; the specific goals of which are to obtain pain relief by providing decompression of the nerves, optimizing spinal balance, and achieving a solid fusion. In many cases, these patients require treatment strategies that address both the front and back of the spinal column to release the spine and make it more flexible and then correct the deformity and lock it in place.
Traditional approaches to accomplish this task have involved surgery through the abdomen to obtain access to the front of the spine, followed by a surgery from the back. These interventions have been associated with not only large unsightly scars but a complication risk ranging between 30 and 80%. As the contemporary treatment of this condition has evolved, spine surgeons have employed numerous strategies to minimize those risks—the incorporation of minimally invasive spinal techniques is the most recent of such innovations.
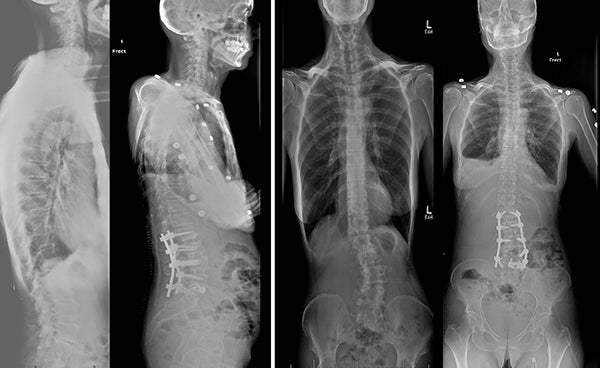
Surgery for adult scoliosis is now performed at UPMC in a staged fashion. A posterior approach is initially performed to remove the rigid bones that have grown across the joints while decompressing the nerve roots and restoring flexibility to the spinal column. After a few days, stage 2 is performed employing minimally invasive techniques (i.e., XLIFs) to gain lateral access to the disc spaces in the front of the spine. The collapsed discs are removed and replaced with height restoring cages and biologic agents to enhance the nerve root decompression and augment spinal realignment. This approach not only limits the surgical scars, but also the blood loss, pain and many of the complications associated with the large abdominal approaches of years past. Screws and rods are then placed through the initial incision in the back to finalize the deformity correction and fortify the final structure and position of the spine.
We have developed a unique, multi-staged approach to the surgical treatment of the very complex and all too often incapacitating condition of adult degenerative scoliosis. We continue to gather data and employ scientific prudence while treating every patient as an individual with a unique set of needs, employing contemporary surgical techniques at the forefront of innovation and practice.